Nutrition
How do critically ill or injured patients receive nutrition?
Due to a critical illness or injury, some ICU patients cannot eat in the usual fashion. Therefore, nutrition is often given to patients in the ICU through feeding tubes or intravenously. The preferred way to provide nutrition to ICU patients is through the feeding tube. However not all ICU patients can receive nutrition through a feeding tube and they must be fed intravenously.
How are tube feedings given?
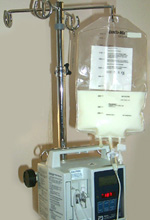
Liquid tube feedings may be given to patients through nasogastric, nasoduodenal, gastrostomy, or jejunal tubes. These tubes provide access to the stomach or small intestines for feeding. Tube feeding may be given through these tubes at a constant rate over a twenty-four hour period or by specific amounts given periodically through a twenty-four hour period. Often a feeding pump is used to assure that the specified amount of tube feeding is delivered over the twenty-four hour period. Liquid tube feedings are typically seen at the bedside hanging from an IV pole infusing through the feeding pump. The tube feeding solution is usually changed or adjusted every twenty-four hours.
What type and how much tube feeding is given?
A number of tube feeding products are available. The doctor, dietician, pharmacist, and nurse will help to decide what each individual patient requires. Fortunately liquid tube feedings are very complete and include: protein, fat, carbohydrates, and vitamins. Recently, specialized tube feedings have become available that enhance the healing of ICU patients with certain conditions. If you have further questions regarding nutritional issues you should talk to the nurse or doctor.
Do tube feedings hurt?
Tube feedings usually do not hurt and most ICU patients do not realize that they are receiving tube feedings unless they are told. Occasionally patients may develop cramping, diarrhea or nausea when receiving liquid tube feedings.
How long are tube feedings needed?
Tube or intravenous feedings are necessary until the patient is able to consume appropriate amounts of nutrition by eating.
When and how are intravenous feedings given?
Intravenous feedings are given to patients who are unable to tolerate tube feedings. The medical staff will refer to intravenous feedings as TPN (total parenteral nutrition) or PPN (peripheral parenteral nutrition). TPN must be given through a central venous catheter and the PPN may be given through a regular IV. Similar to tube feedings, the intravenous feeding provides the patient with the complete amount of protein, carbohydrate, aft, and vitamins. Intravenous feeding will be seen at the bedside hanging from an IV pole infusing through an IV pump. If the intravenous feeding has fat added to it, it will look white.
Does intravenous feeding hurt?
Intravenous feeding does not hurt and patients do not know if they are receiving it unless they are told.
Are there any potential complications associated with use of intravenous feedings?
The doctor, dietician, pharmacist, and nursing staff will closely monitor patients receiving intravenous feedings. Electrolytes, liver function, and glucose may be effected in patients receiving intravenous feeding. Not uncommonly, a patient's glucose will be temporarily elevated while receiving intravenous feeding and they may require treatment for the elevated glucose including insulin. This may occur in patients who are not known to be diabetic.
Feeding tube (black arrow)
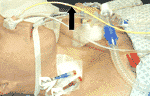
Intravenous feeding (total parenteral nutrition - TPN)